
Polycystic kidney disease. POLYCYSTIC KIDNEY DISEASE OVERVIEWNormally, the kidneys filter out excess toxic and waste substances and fluid from the blood. In people with polycystic kidney disease (PKD), the kidneys become enlarged with multiple cysts that interfere with normal kidney function. This can sometimes lead to kidney (renal) failure and the need for dialysis or kidney transplantation. There are two major forms of PKD: autosomal dominant polycystic kidney disease (ADPKD) and autosomal recessive polycystic kidney disease (ARPKD). Autosomal dominant means that each child of an affected parent has a 5. In addition, autosomal dominant means that it does not skip generations (ie, if a patient with the disease does not pass it along to one of his or her children, then the disease disappears from that family and grandchildren cannot inherit the disease). However, some patients with ADPKD are not diagnosed during their lifetimes, due to very few symptoms. 
This means that a family member may have the disease without knowing it. The estimated incidence is approximately 1 in 2. Autosomal recessive means that the mutated gene must be present in both parents, who, because they carry one abnormal gene, are considered carriers. When both parents are carriers (each having one abnormal and one normal gene), there is a 2. The following is a discussion of ADPKD, the most common polycystic kidney disease. GENETICS OF AUTOSOMAL DOMINANT POLYCYSTIC KIDNEY DISEASEApproximately 8. ADPKD) have a mutation in the PKD1 gene, located on chromosome 1. PKD1 disease. The remaining 1. PKD2 gene on chromosome 4; this is called PKD2 disease. In some cases, it is not possible to detect which gene is mutated. PKD2 disease is milder; therefore, it often presents later in life and is sometimes not diagnosed at all. Thus, it is likely that more than 1. ADPKD have PKD2 disease. Kidney failure occurs at an earlier age in PKD1 patients; the average age of end- stage renal disease (ESRD; that is, needing dialysis or a transplant) is approximately 5. PKD1 versus 7. 4 years in PKD2 patients. 
Everything NICE has said on chronic kidney disease (renal failure) in an interactive flowchart.In approximately 1. ADPKD occurs in people without a family history of the disease (ie, family members have been evaluated and have no evidence for PKD). This is due to the patient having a new (de novo) genetic mutation that was not present in either parent. CYST FORMATIONAutosomal dominant polycystic kidney disease (ADPKD) appears to cause abnormal cell growth that leads to cysts on the kidneys. The basic unit of the kidney is the nephron, with each kidney containing approximately one million nephrons (figure 1 and figure 2). Each nephron consists of a glomerulus, which is a collection of very small arteries intermingled among a series of tubules. The glomeruli and tubules work together to filter waste products from the bloodstream and dispose of them in the urine. In ADPKD, cyst formation begins as an expansion, or ballooning, of a tubule in a small proportion of nephrons. The cyst subsequently enlarges, usually due to fluid secretion into the cyst. The cells making up the cysts multiply, causing the cyst to grow even larger. Kidney disease (renal disease) in dogs and cats may cause symptoms including increased drinking and urinating, loss of appetite, and depression. Kidney Damage Stage Reduced! Stage 3 Reduced to Stage 2 Kidney Disease.  
Third Stage Kidney Disease. Third stage kidney disease is moderately serious, but offers number of treatment options. Read on to know more. Chronic kidney disease symptoms. Chronic kidney failure, as opposed to acute kidney failure, is a slow and gradually progressive disease. Even if one kidney stops. 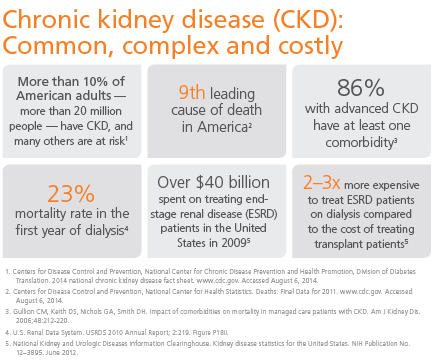
Cysts may also grow in other organs, including the liver, pancreas, thyroid gland, and/or spleen. EFFECTS ON THE KIDNEYAutosomal dominant polycystic kidney disease (ADPKD) often leads to progressive kidney (renal) failure due primarily to continued enlargement of the cysts and replacement of normal kidney tissue. Other problems involving the kidney can occur, including high blood pressure, kidney infection, blood in the urine (hematuria), and kidney stones. Flank and abdominal pain are also common. Kidney failure — Kidney (renal) failure severe enough to require dialysis or kidney transplantation is called end- stage renal disease (ESRD). ADPKD rarely leads to ESRD in early childhood; it most commonly occurs in middle age or later in life. The likelihood of requiring dialysis in people with ADPKD is estimated at less than 2 percent in people under age 4. Not all patients with ADPKD develop kidney failure, particularly those with PKD2. As an example, having enlarged kidneys is the most reliable predictor for developing renal failure in patients with ADPKD. In addition, factors that increase the risk of developing kidney failure include being male, having PKD1 disease, having episodes of visible blood or detectable protein in the urine, or having high blood pressure (particularly before age 3. 8 Diet and Nutrition Goals for People with Stage 3 Chronic Kidney Disease. In stage 3 chronic kidney disease (CKD), the kidneys still function sufficiently to remove. Enlarged kidneys or increased total kidney volume due to a high cyst burden is associated with all of these complications and is the most important risk factor for progression to renal failure. High blood pressure — High blood pressure is a common feature of ADPKD, occurring in 6. Over 9. 0 percent of patients will have high blood pressure by the time they reach end- stage renal failure. Men have higher blood pressures than women, and high blood pressure is associated with bigger kidneys and faster rates of kidney growth. The primary symptoms of a kidney infection in people with ADPKD are fever and flank pain. The infection may be of the kidney or of a cyst. Not all antibiotics work well if the infection is in the cyst. Since it is not easy to tell where the infection is, most physicians will use an oral antibiotic that can penetrate into the cyst cavity. Some people with high fevers or severe symptoms need to be treated with intravenous antibiotics. The duration of treatment for a cyst or kidney infection is typically longer than with a routine kidney infection in someone without ADPKD. With hematuria, the urine may be a pink or red color. Repeated episodes of hematuria are common. 
Hematuria is associated with increased kidney size and a faster rate of kidney growth. This can occur as a result of strenuous activity, and bleeding can cause pain in the side of the low back (called flank pain). Patients with ADPKD can also develop kidney stones, which can cause hematuria and flank pain. Hematuria related to bleeding cysts generally stops within two to seven days. The usual treatment includes bed rest and increasing fluids until the bleeding stops. If bleeding does not stop with bed rest and increased fluids, a procedure to stop the bleeding may be required. Bleeding into a cyst that does not communicate with the urinary system may not produce visible blood; in this setting, patients typically have localized flank pain and, in some cases, a low- grade fever. Kidney stones — Kidney stones occur in up to 2. ADPKD. Kidney stones may cause pain, or sometimes they can block the flow of urine without symptoms. Treating kidney stones that block urine flow is extremely important in patients with ADPKD. If the blockage is not relieved, the function in that kidney may be lost. Relieving the blockage may require the help of a urologist. The cysts make it harder to surgically remove the stone or use shock waves to break up the stone (extracorporeal shock- wave lithotripsy . People with ADPKD often develop flank and abdominal pain that is not related to infection, bleeding into a cyst, or a kidney stone. The pain is often dull and persistent and is thought to be caused by stretching of the wall of a cyst or pressure on other organs when the kidneys and/or liver are very large. This is the most common symptom in ADPKD patients. In contrast, pain that begins suddenly is more likely to be caused by bleeding into or infection of a cyst, twisting of the kidney, or a kidney stone. No specific treatment is required in most people with dull or persistent flank and abdominal pain; pain medications such as acetaminophen are often recommended. The use of nonsteroidal anti- inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, is not recommended, although people with ADPKD may, on occasion, benefit from these medications and should speak to their healthcare provider about the risks and benefits of NSAIDs before using them. NSAIDs are not recommended for patients with ADPKD when kidney function is reduced or when they need to be used on a long- term basis to treat chronic pain basis. Some people have persistent pain that is severe enough to limit their daily activities. Severe pain is usually evaluated with renal imaging to see if a large cyst is present in the area of pain. If so, a needle through the skin can be used for drainage of the cyst. This needs to be done with appropriate imaging and a radiologist who is trained in this type of technique. Most people have significant relief of pain after drainage. However, pain can recur, and surgery is sometimes required to relieve chronic pain that interferes with quality of life. ASSOCIATION CONDITIONS OUTSIDE OF THE KIDNEYA variety of conditions outside the kidney can occur in people with autosomal dominant polycystic kidney disease (ADPKD). These conditions can involve a number of systems, including the liver, vascular system, and the connective tissue. Intracranial aneurysm — The most serious possible complication of PKD is a cerebral or brain aneurysm (a bulging blood vessel due to weakening of the blood vessel wall). Aneurysms can rupture, causing bleeding into the brain (subarachnoid hemorrhage). If not treated before the aneurysm ruptures, this can lead to irreversible brain damage or death. Aneurysm rupture occurs most often in people with larger aneurysms (> 1. The most common symptom of subarachnoid hemorrhage is a severe headache that begins suddenly, often with a pop, frequently with nausea and vomiting. Compared with the general population, the risk of developing an aneurysm in ADPKD is approximately fivefold greater. People with a first- degree relative with a history of intracranial aneurysm or subarachnoid hemorrhage are at the highest risk of forming an aneurysm. Early detection (before symptoms occur) of intracranial aneurysms is recommended in people who are at high risk. Screening (looking for an aneurysm before it ruptures) is generally performed with magnetic resonance angiography (MRA) or, if not available, a computed tomography (CT) scan.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2017
Categories |
 RSS Feed
RSS Feed
